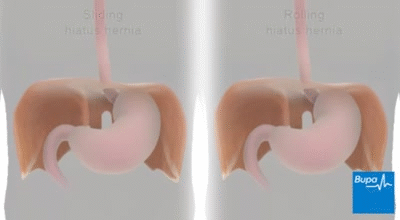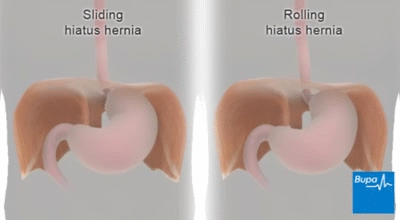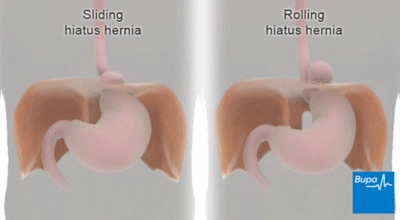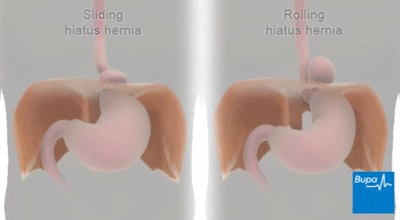
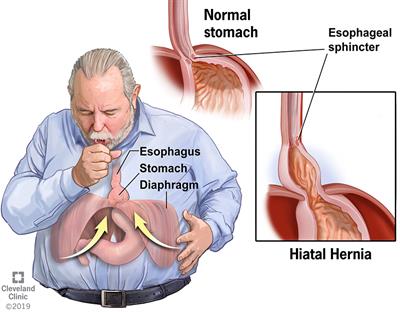
A hiatal hernia occurs when the upper part of your stomach bulges through the large muscle separating your abdomen and chest (diaphragm).
Your diaphragm has a small opening (hiatus) through which your food tube (esophagus) passes before connecting to your stomach. In a hiatal hernia, the stomach pushes up through that opening and into your chest.
A small hiatal hernia usually doesn’t cause problems. You may never know you have one unless your doctor discovers it when checking for another condition.
But a large hiatal hernia can allow food and acid to back up into your esophagus, leading to heartburn. Self-care measures or medications can usually relieve these symptoms. A very large hiatal hernia might require surgery.
Symptoms
Most small hiatal hernias cause no signs or symptoms. But larger hiatal hernias can cause:
- Heartburn
- Regurgitation of food or liquids into the mouth
- Backflow of stomach acid into the esophagus (acid reflux)
- Difficulty swallowing
- Chest or abdominal pain
- Feeling full soon after you eat
- Shortness of breath
- Vomiting of blood or passing of black stools, which may indicate gastrointestinal bleeding
When to see a doctor
See your doctor if you have any persistent signs or symptoms that worry you.
Causes
A hiatal hernia occurs when weakened muscle tissue allows your stomach to bulge up through your diaphragm. It’s not always clear why this happens. But a hiatal hernia might be caused by:
- Age-related changes in your diaphragm
- Injury to the area, for example, after trauma or certain types of surgery
- Being born with an unusually large hiatus
- Persistent and intense pressure on the surrounding muscles, such as while coughing, vomiting, straining during a bowel movement, exercising or lifting heavy objects
Risk factors
Hiatal hernias are most common in people who are:
- Age 50 or older
- Obese
If you experience heartburn and acid reflux, your doctor may recommend:
- Antacids that neutralize stomach acid. Antacids, such as Mylanta, Rolaids and Tums, may provide quick relief. Overuse of some antacids can cause side effects, such as diarrhea or sometimes kidney problems.
- Medications to reduce acid production. These medications — known as H-2-receptor blockers — include cimetidine (Tagamet HB), famotidine (Pepcid AC) and nizatidine (Axid AR). Stronger versions are available by prescription.
- Medications that block acid production and heal the esophagus. These medications — known as proton pump inhibitors — are stronger acid blockers than H-2-receptor blockers and allow time for damaged esophageal tissue to heal. Over-the-counter proton pump inhibitors include lansoprazole (Prevacid 24HR) and omeprazole (Prilosec, Zegerid). Stronger versions are available in prescription form.
Surgery
Sometimes a hiatal hernia requires surgery. Surgery is generally used for people who aren’t helped by medications to relieve heartburn and acid reflux, or have complications such as severe inflammation or narrowing of the esophagus.
Surgery to repair a hiatal hernia may involve pulling your stomach down into your abdomen and making the opening in your diaphragm smaller or reconstructing an esophageal sphincter. In some cases, hiatal hernia surgery is combined with weight-loss surgery, such as a sleeve gastrectomy.
Surgery may be performed using a single incision in your chest wall (thoracotomy) or using a minimally invasive technique called laparoscopy. In laparoscopic surgery, your surgeon inserts a tiny camera and special surgical tools through several small incisions in your abdomen. The operation is then performed while your surgeon views images from inside your body that are displayed on a video monitor.
Leave a comment